Photo: Yahoo Finance
Have you watched from the sidelines as investors (neighbors, friends, family, etc.) invest money into the stock market and brag about their returns? How does a person invest? Which stocks do you choose? How do you avoid paying all your returns to the broker as fees? I will tell you a simple method to start with.
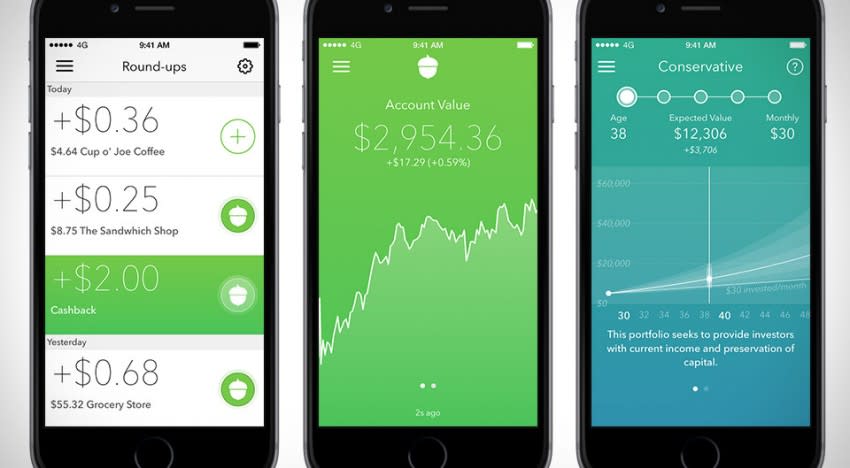
Acorn investing services are a great way to start investing in the stock market. I was super skeptical of the process at first. However, then a fellow staff member at my work convinced me to just start with the basic process of the service. Which is?
Investing made easy!
To start with, follow the link to Acorns here:
Note: I do get credit for referring you.
But more importantly, connecting your checking account to the Acorns account will allow the service to withdraw small amounts of money. I mean small donations - rounding up your purchases to a $1. That means, say, you spend $0.75 on a purchase. Then Acorns will invest $0.25 into the stock market in your Acorns account.
Small Amounts Add Up Quickly - well relatively so
Don't expect to get rich overnight. But I have been with the service for 4 years and looked at my account the other day. I was pleasantly surprised to see that I had a balance of $4,000. Wow! An average return of 20-30% on my deposits.
You don't have to believe me. But I will continue to use the service to build money without having to look at the account. I have not looked at the account for 4 years.
Note: If you withdraw money from the account, you will pay taxes on capital gains as profits.
I suggest that you take advantage of this service. It is cheap as far as fees are concerned. Plus, compare the returns (profits) to your brokerage accounts (retirement, 401K, etc.). Acorns will outperform some of these with computerized (AI) investing.
Note: I set my risk level on Acorns to 'Aggressive' = I want the largest return. I am willing to risk some change.